What are the causes of Cauda Equina Syndrome
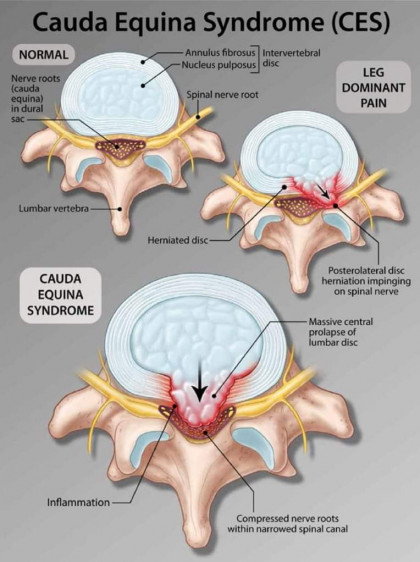
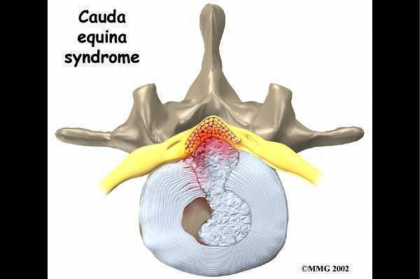
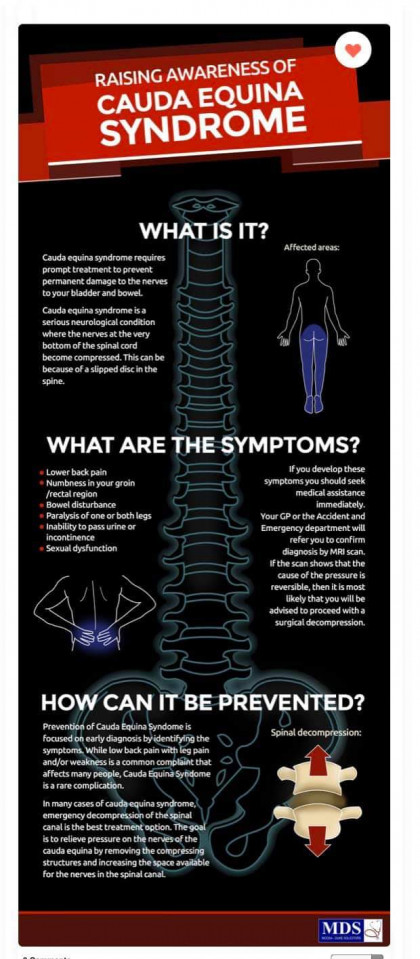
Cauda Equina Syndrome occurs when the bundle of nerves in the lower spine are compressed resulting in neurological symptoms. Typically, pressure on the spinal nerves is caused a by either a severely herniated lumbar disc or a collection of fluid, usually blood, around the base of the spine following a surgical procedure. Although the cause of Cauda Equina Syndrome can vary, the treatment is the same — Alleviate the pressure on the nerve roots as soon a medically possible.
In the situation where Cauda Equina Syndrome is the result of a severely herniated lumbar disc, most often the patient will present to a hospital emergency department with complaints of sudden and severe back pain. What differentiates a patient with Cauda Equina Syndrome verses a non-emergent condition, such as sciatica, is a complaint of urinary dysfunction of either incontinence or retention. A finding or complaint of urinary dysfunction should result in a full neurological work-up including a stat MRI of the lumbar spine followed by a consultation with the on-call neurosurgeon. A confirmed diagnosis of Cauda Equina Syndrome should be treated as a surgical emergency, and surgery to decompress the nerve roots by removing the offending disc material should be performed as soon as medical possible and within 48 hours of the onset of symptoms.
Where Cauda Equina Syndrome is the caused by a post-surgical hematoma on the spine, the diagnosis may be more subtle. Specifically, much like the herniated disc, the hematoma will compress the nerve roots which will result in urinary dysfunction. However, urinary dysfunction may not be easily diagnosed in the surgical setting because the patients are typically catheterized. In such cases, it is incumbent on the post surgical medical team to closely monitor the patient for atypical symptoms such as unusually intense post surgical pain and laboratory results suggestive of internal bleeding. If a hematoma induced Cauda Equina Syndrome is suspected, the patient should undergo a stat MRI of the lumbar spine followed by a consultation with the surgeon. A confirmed diagnosis of Cauda Equina Syndrome should be treated as a surgical emergency, and surgery to decompress the nerve roots by evacuating the hematoma should be performed as soon as medical possible and within 48 hours of the conclusion of the first surgery.